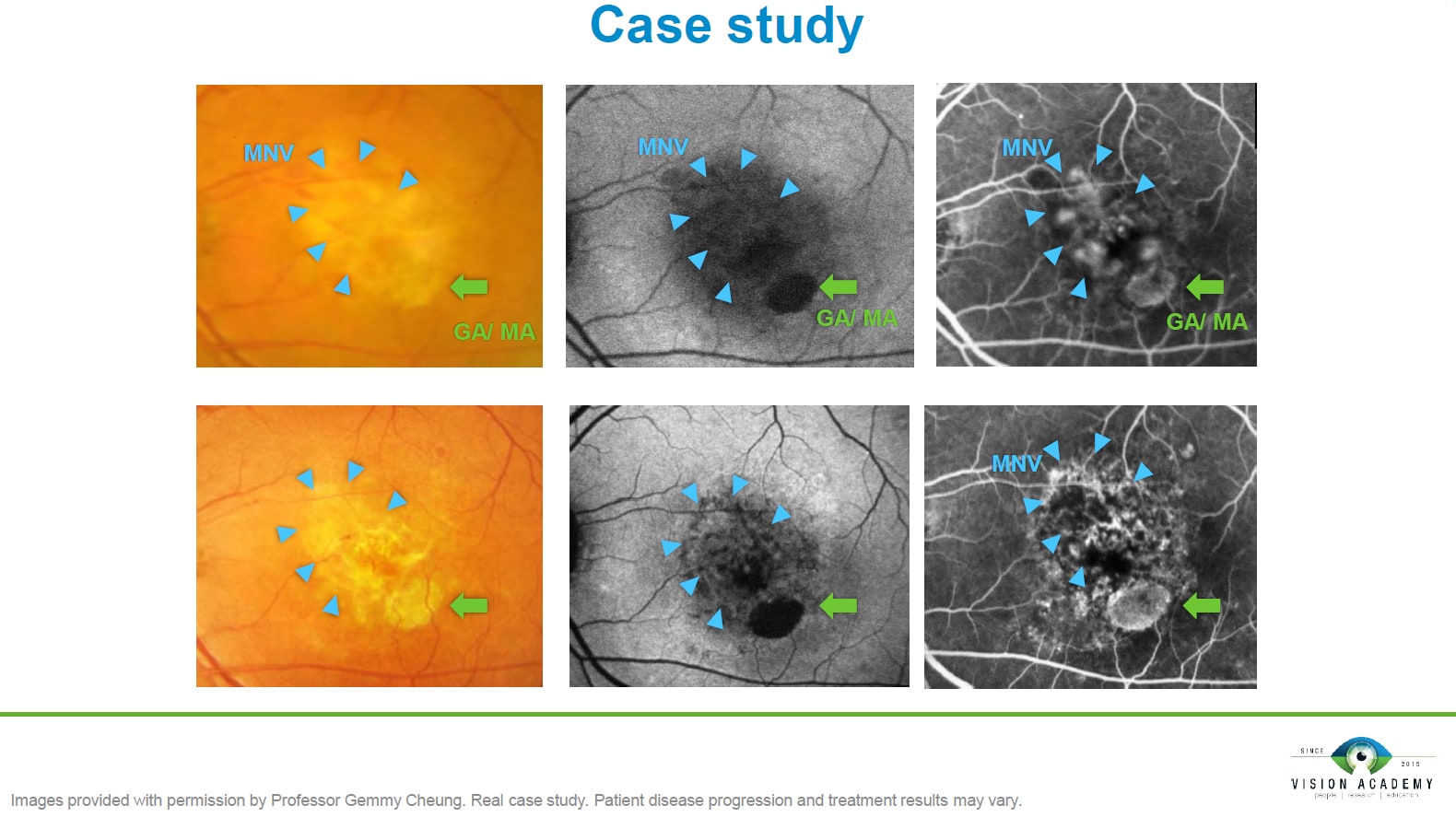
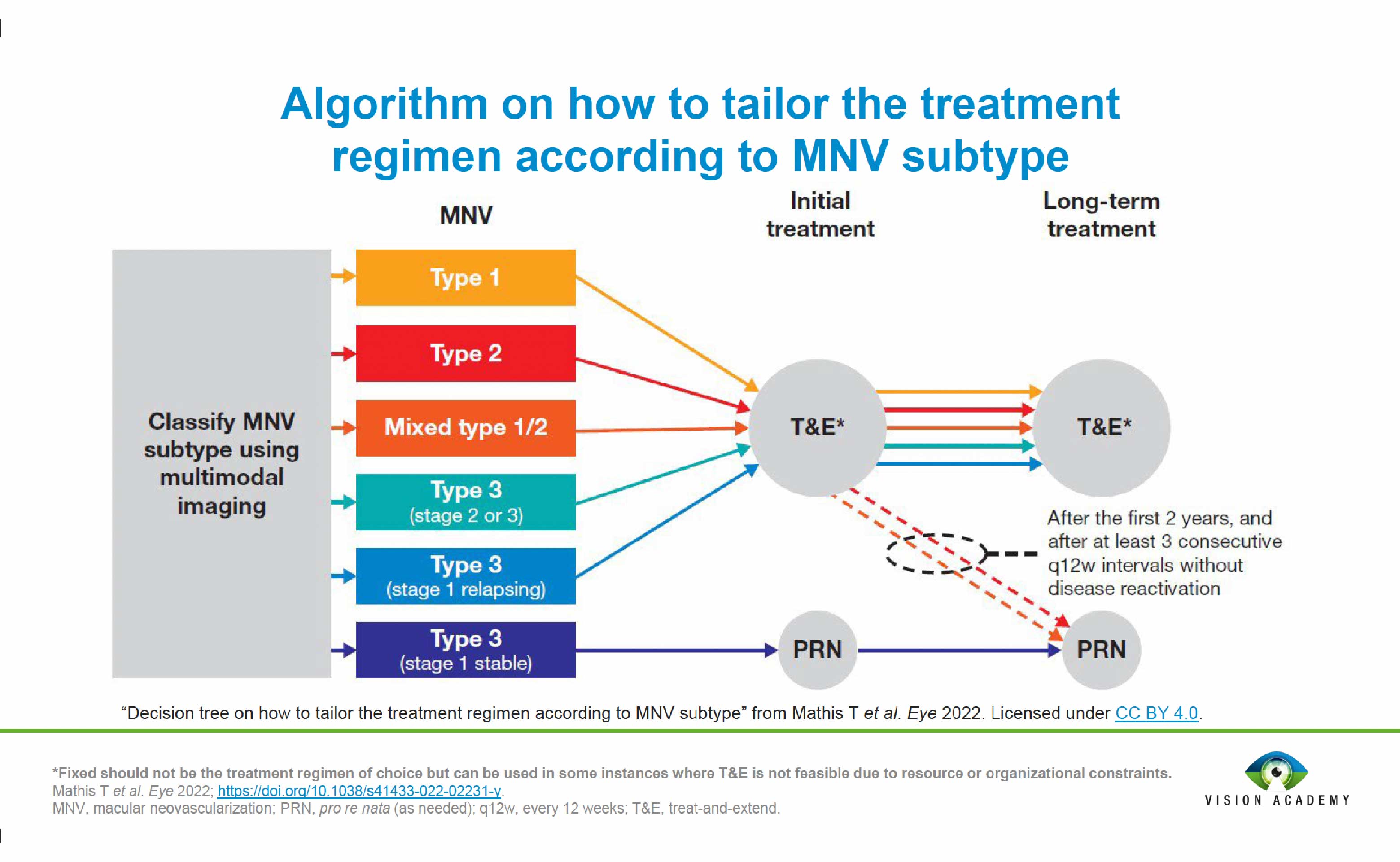
nAMD is not a uniform disorder, as different subtypes of MNV have different characteristics and prognoses. This partly explains why patients respond differently to treatment according to disease characteristics. Defining and differentiating MNV subtypes is important in the management of nAMD to ensure optimal response to treatment. A clearly defined classification of MNV provides information on prognosis, thereby facilitating patient management.
The Vision Academy has provided expert consensus on the definitions and characteristics of MNV subtypes, as well as recommendations for differentiating between and tailoring treatment to specific subtypes.
Challenging clinical situations
Through collective expertise in areas with insufficient conclusive evidence, we seek to provide guidance on best clinical practice in key areas: